11 Early Warning Signs Of Prediabetes Most People Miss — How To Spot Them Before It’s Too Late
Prediabetes is a quietly growing health problem: millions of people have it and don’t know. Left unchecked, it often progresses to type 2 diabetes, with increased risk for heart disease, nerve damage, and vision loss. We want to help you recognize the early warning signs that most people, and even many clinicians, miss. Early detection changes everything: it gives us a chance to reverse metabolic decline with lifestyle changes, targeted treatment, and close monitoring. In this text we’ll walk through 11 specific, sometimes subtle clues that suggest rising blood glucose or insulin resistance. For each sign we explain why it happens, how to spot it in everyday life, and what concrete next steps to take. Read on, catching these signals now can save years of complications later.
Why Early Detection Of Prediabetes Changes Everything
Early detection of prediabetes isn’t just medical nitpicking: it’s a clinical pivot point. Once we recognize metabolic dysfunction early, we can literally reverse or delay progression with interventions that are evidence-based and scalable. Trials like the Diabetes Prevention Program (DPP) showed that structured lifestyle changes, weight loss of 5–7% and 150 minutes of weekly moderate activity, cut progression to diabetes by about 58% over three years. That’s not hypothetical: it’s powerful, real-world impact.
Why does timing matter? Prediabetes represents a period of metabolic instability: insulin resistance is increasing, pancreatic beta cells are under stress, and subtle vascular changes begin. Intervening here means less cumulative exposure to high glucose and fewer microvascular and macrovascular insults. Clinically, early detection lets us tailor risk reduction: prioritize diet and exercise, address sleep and stress, optimize blood pressure and lipids, and consider medications like metformin in high-risk patients.
From a public-health perspective, detecting prediabetes early lightens the downstream burden on hospitals and health systems, reduces medication needs, and preserves quality of life. For individuals, catching it early means fewer pills, more agency, and a better chance of keeping diabetes at bay. That’s why recognizing even subtle signs, our next 11 clues, matters so much.
Subtle Metabolic Clues: High Blood Pressure, Abnormal Lipids, And Elevated Waist Measurement
Prediabetes rarely appears alone. It often accompanies a cluster of metabolic changes, high blood pressure, atherogenic lipid patterns, and increased abdominal fat, collectively called metabolic syndrome. These signs can be easier to spot than a fasting blood glucose that’s only slightly elevated.
High blood pressure: We should watch for sustained readings at or above 130/85 mmHg. Insulin resistance raises sympathetic tone and sodium retention, contributing to higher pressures. If you’ve noticed creeping BP readings at clinic visits or home monitoring, that’s a red flag.
Abnormal lipids: Look for elevated triglycerides and low HDL cholesterol, sometimes total cholesterol looks “okay,” but the triglyceride-to-HDL ratio tells a different story. A fasting triglyceride above 150 mg/dL or an HDL below 40 mg/dL (men) or 50 mg/dL (women) frequently accompanies insulin resistance.
Waist measurement: Waist circumference is a simple, powerful tool. For many populations, measures above ~35 inches (women) and ~40 inches (men) correlate with visceral fat and higher metabolic risk. We can measure at the top of the hip bones or the narrowest waist, consistency matters.
Taken together, these clues suggest systemic metabolic dysfunction even when fasting glucose is borderline. If we observe this triad, we should push for glucose testing (fasting glucose, HbA1c, or an oral glucose tolerance test) and intervene early with lifestyle changes and close follow-up.
Increased Thirst And Frequent Urination: The Classic Early Signal
Polyuria (frequent urination) and polydipsia (increased thirst) are classic symptoms of hyperglycemia, and they can appear even in prediabetes when glucose spikes are intermittent. When blood glucose exceeds the renal threshold, typically around 180 mg/dL, glucose spills into the urine, pulling water with it and increasing urine output. That leads to dehydration signals: dry mouth and stronger thirst.
We often dismiss these symptoms as simple dehydration or caffeine effects. But persistent patterns, needing to get up at night to urinate more frequently, feeling thirsty all day even though drinking water, or noticing heavier fluid intake, warrant attention. Pay attention to nocturia (nighttime urination): it’s a common early complaint that disrupts sleep.
How to evaluate: Check a fasting glucose or HbA1c, and if those are borderline, consider a random glucose or 2-hour oral glucose tolerance test (OGTT) to catch post-meal spikes. A simple urine dipstick showing glucosuria is another diagnostic hint.
Immediate actions: Drink water, avoid sugary drinks, and note the pattern (when symptoms occur relative to meals or alcohol). If the symptoms are recurring, schedule testing and discuss early interventions, dietary adjustments that reduce post-meal glucose surges and increasing physical activity can blunt these episodes quickly.
Unexplained Fatigue, Low Energy, And Brain Fog
Feeling drained, sluggish, or unfocused isn’t just about bad sleep or overwork, metabolic dysfunction can sap energy in subtle ways. Insulin resistance alters how tissues use glucose: cells that ought to receive steady fuel become inefficient, which can manifest as chronic fatigue, low exercise tolerance, and cognitive fog.
We hear from patients who say they’re mentally slower, have trouble concentrating through the afternoon slump, or rely on multiple cups of coffee to get through the day. These complaints are easy to dismiss, but when paired with other risk markers they point toward early metabolic trouble.
Mechanisms: High insulin and fluctuating glucose levels affect brain function, glucose spikes can be followed by reactive hypoglycemia, creating short-lived energy crashes. Chronic low-grade inflammation associated with insulin resistance also affects neurotransmitter balance and motivation.
What to do: Start with simple tracking. Keep a 1–2 week diary logging energy levels, sleep quality, meal times, and carbohydrate intake. Note patterns, do symptoms worsen after carb-heavy meals or late-night snacks? Interventions that improve insulin sensitivity, moderating carbohydrate portions, prioritizing protein and fiber, and including brief post-meal walks, often yield noticeable energy improvements within days to weeks. If fatigue persists even though lifestyle changes, investigate other causes (thyroid function, iron deficiency, sleep apnea) with your clinician.
Persistent Hunger And Difficulty Losing Weight, Especially Around The Belly
One paradox of prediabetes: people can be hungry all the time yet struggle to lose weight, especially abdominal fat. Insulin’s role as a storage hormone means that when insulin levels are chronically elevated, the body favors fat storage and makes weight loss harder even though calorie-conscious efforts.
Persistent hunger: We might feel unsatiated after meals, crave carbohydrates or sweets, or experience frequent mid-afternoon hunger. This isn’t merely willpower, physiological insulin signaling and altered hunger hormones like leptin and ghrelin are at play.
Difficulty losing weight: Standard diet-and-exercise approaches sometimes produce smaller-than-expected results for people with insulin resistance. The key is tailoring strategies that reduce hyperinsulinemia: lower glycemic load meals, time-restricted eating for some individuals, and resistance training to build muscle mass and improve glucose uptake.
Central obesity: Visceral fat, fat around the organs, releases inflammatory cytokines and worsens insulin resistance. That’s why waist circumference is a stronger predictor of metabolic risk than BMI for many people. If you or someone you care for notices stubborn belly fat even though efforts, that’s a practical signal to test for prediabetes.
Practical steps: Focus on protein-rich breakfasts, increase fiber (vegetables, legumes), prioritize resistance and high-intensity interval training twice weekly, and consider consulting a dietitian for individualized plans. Small, sustainable shifts often yield better long-term outcomes than short, restrictive diets.
Skin And Wound Problems: Acanthosis Nigricans, Slow Healing, And Recurrent Infections
Our skin often gives early metabolic clues. Acanthosis nigricans, velvety, darkened patches typically found on the back of the neck, armpits, or groin, is strongly associated with insulin resistance. It’s not cosmetic fluff: it’s a dermatologic marker of systemic metabolic stress.
Slow healing and recurrent infections: Elevated glucose levels impair immune function and reduce tissue repair capacity. That means cuts, scrapes, and insect bites may take longer to heal, and fungal or bacterial skin infections (including warm, moist areas like under breasts or in skin folds) can recur.
Yeast overgrowths like candidiasis present with itching, redness, and sometimes white discharge in body folds or the genitals, these can be early pointers to elevated glucose in tissues. Similarly, persistent athlete’s foot or recurrent nail infections warrant metabolic screening if they occur alongside other risk features.
What to look for: Examine the neck for darkened, coarse patches: notice whether small wounds take weeks rather than days to close: track recurrent fungal infections even though standard topical treatments. If you find these patterns, get glycemic testing and make skin-care adjustments: keep areas dry, manage weight, and optimize blood sugar through diet and activity.
Referral: For acanthosis nigricans, a dermatology consult can confirm the diagnosis and help rule out rarer causes, but its presence should prompt metabolic evaluation first and foremost.
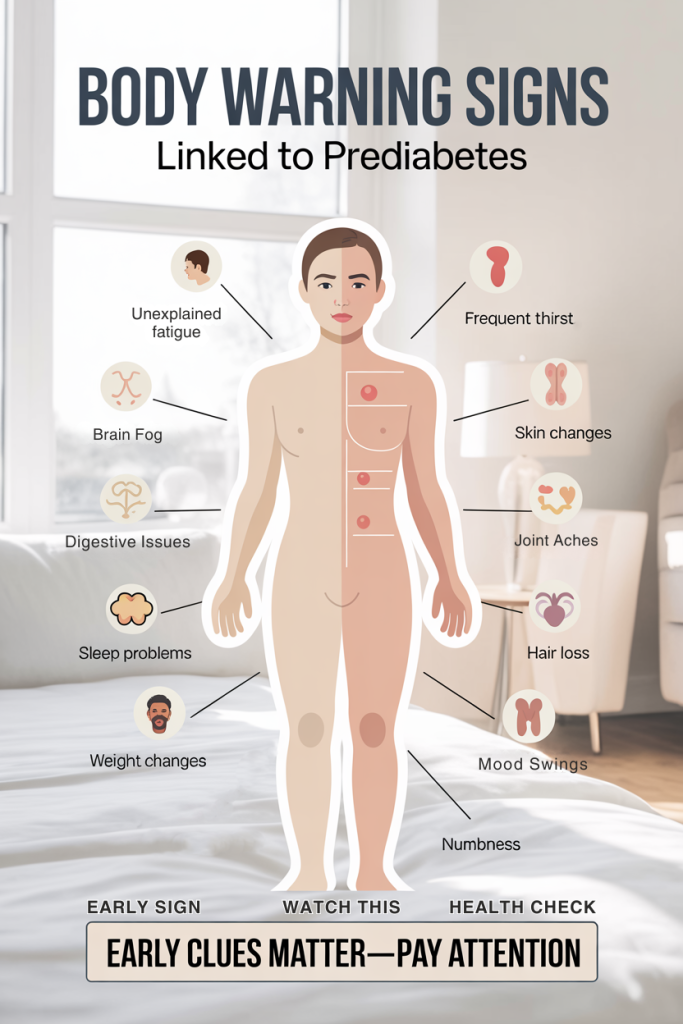
Numbness, Tingling, Or Burning In Hands Or Feet (Early Neuropathy Signs)
Peripheral neuropathy is often thought of as a late complication of diabetes, but nerve symptoms can begin during prediabetes. Small fiber neuropathy, painful burning, tingling, or numbness in the toes, feet, or hands, may be an early indicator of metabolic nerve injury.
Presentation: Symptoms can be intermittent at first, worse at night or with certain footwear, and may be dismissed as “pinched nerves” or aging. Because these sensations impact quality of life and function, recognizing the metabolic contribution is important.
Mechanism: Chronically elevated glucose and insulin resistance cause microvascular changes and oxidative stress that damage small nerve fibers. Low-grade inflammation contributes as well.
Assessment: A focused neurologic exam, monofilament testing for protective sensation, and vibration testing help quantify dysfunction. Some clinics use skin biopsy or specialized nerve testing for small-fiber neuropathy when diagnosis is unclear.
Management: Early intervention matters. Improving glycemic control and addressing metabolic risk factors can slow or sometimes reverse early neuropathic symptoms. Pain management strategies, topical agents, gabapentinoids, or SNRIs, can provide symptomatic relief while metabolic interventions take hold. We recommend prompt evaluation if you notice persistent tingling, burning, or unexplained numbness.
Vision Changes And Oral Health Issues: Blurred Vision And Gum Disease
Elevated glucose affects tissues throughout the body, including the eyes and mouth, often earlier than we expect. Blurred vision that fluctuates over days to weeks can result from transient changes in lens hydration when blood glucose varies. It’s not always a permanent refractive error: sometimes it’s a metabolic signal.
Oral health: Gum disease (periodontitis) and recurrent oral infections show up frequently in people with impaired glucose metabolism. High glucose levels in saliva and periodontal tissues favor bacterial growth and chronic inflammation. In turn, periodontal disease worsens glycemic control, creating a bidirectional relationship.
What to watch for: Sudden or intermittent blurring of near or distance vision, new floaters, or prolonged red/irritated eyes should prompt timely eye evaluation and glycemic testing. In the mouth, persistent bleeding gums, loosened teeth, chronic bad breath, or slow-healing sores are warning signs.
Action steps: Schedule comprehensive dental and eye exams if these issues arise. Dentists and optometrists often detect metabolic clues during routine visits and can recommend glucose testing. Good oral hygiene, smoking cessation, and improved glycemic control can markedly reduce progression of periodontal disease and protect vision over time.
Less-Obvious Clues: Sexual Dysfunction, Yeast Infections, And Frequent Yeast Overgrowth
Some signs of prediabetes are intimate and rarely discussed, but they matter. Sexual dysfunction, erectile dysfunction in men and decreased sexual interest or lubrication problems in women, can be an early consequence of vascular and neurologic changes from impaired glucose metabolism. Erectile dysfunction, in particular, often predates cardiac events and should trigger metabolic evaluation.
Recurrent yeast infections: As noted earlier, Candida thrives in glucose-rich environments. Women who experience frequent vaginal yeast infections or men with persistent genital yeast should consider glucose screening. Yeast overgrowth may present with itching, burning, and white discharge and often resists single-course treatments if underlying glucose is unchecked.
Menstrual irregularities and PCOS overlap: Polycystic ovary syndrome (PCOS) is strongly linked to insulin resistance: irregular periods, acne, and excess hair growth in people with PCOS substantially raise prediabetes risk. We should screen women with PCOS for dysglycemia regularly.
Approach: Because these signs affect quality of life and relationships, address them openly in clinical conversations. Treatment for infections and sexual dysfunction can be started symptomatically, but concurrent metabolic assessment and interventions are essential for long-term resolution. Referral to appropriate specialists, endocrinology, gynecology, urology, may be necessary when symptoms persist.
Conclusion
Recognizing prediabetes early gives us powerful leverage to avert progression and protect long-term health. The 11 signs we’ve outlined, ranging from metabolic cluster features like high blood pressure and abnormal lipids to more subtle clues like skin changes, fatigue, nocturia, and sexual dysfunction, are practical, observable signals that should prompt testing. We don’t want any of these cues dismissed as trivial. If you identify one or more in yourself or someone you care for, take action: measure fasting glucose and HbA1c, discuss an OGTT with your clinician if needed, and prioritize lifestyle strategies shown to reverse risk. Small, consistent changes, improving diet quality, increasing activity, optimizing sleep, and managing stress, often yield outsized benefits. Above all, early detection is an opportunity. Let’s use it.