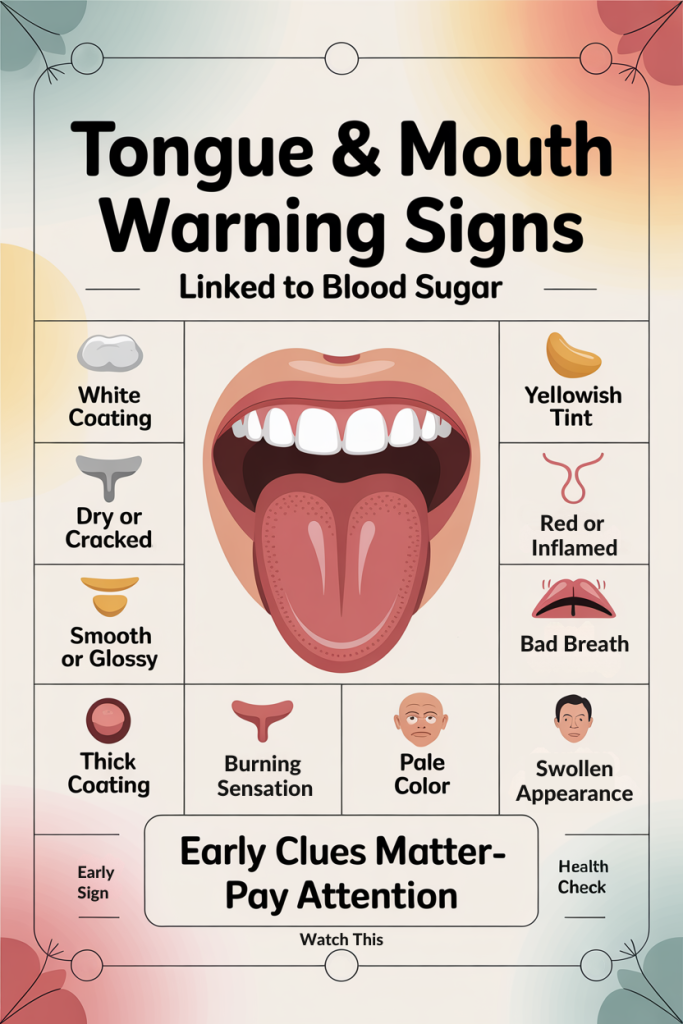
10 Mouth And Tongue Changes Linked To Blood Sugar Problems — What To Watch For
High or unstable blood sugar doesn’t only affect your feet, eyes, and heart, it shows up in the mouth, too. In 2026, with diabetes and prediabetes affecting tens of millions of Americans and more people living longer with metabolic issues, recognizing oral signs can give us an early warning or help us manage complications sooner. In this text we’ll walk through 10 mouth and tongue changes commonly linked to blood sugar problems, explain why they happen, and show what to do if you notice them. Our goal is practical: help you spot changes, understand their connection to glucose control, and take steps, medical and self-care, that protect both your oral health and overall well-being.
Why Blood Sugar Affects Oral Health
High blood glucose and wide glucose swings create an environment that favors infection, inflammation, and poor tissue repair. When we talk about diabetes-related oral health, we’re describing a set of biological effects that make the mouth more susceptible to problems: weakened immune response, higher sugar in saliva that feeds microbes, reduced blood flow that slows healing, and nerve changes that alter sensation.
Immune dysfunction is a big part of the story. Elevated glucose impairs white blood cell function and reduces our ability to fight bacteria and fungi. That’s why periodontal infections are more frequent and more severe in people with poorly controlled blood sugars. At the same time, higher glucose levels in saliva act like fertilizer for certain microbes, Candida, streptococci, and other organisms thrive when more glucose is available.
Reduced salivary flow (dry mouth) and changes in saliva composition also matter. Saliva is our natural cleanser: it buffers acids, clears food debris, and carries antimicrobial proteins. Less saliva means more plaque buildup, more tooth decay, and more infections. Microvascular damage and neuropathy, common in chronic hyperglycemia, reduce nutrient and immune cell delivery to tissues, so small injuries heal slowly and can progress.
Finally, inflammation links systemic metabolic dysfunction to oral disease. Periodontal disease is itself an inflammatory condition that can worsen insulin resistance, creating a two-way street: high blood sugar increases oral disease risk, and severe oral disease can make glycemic control harder. That interplay is why we need to pay attention to mouth and tongue changes as part of metabolic health monitoring.
Dry Mouth (Xerostomia): Causes, Symptoms, And Risks
Dry mouth, or xerostomia, is one of the most common oral complaints among people with blood sugar problems. We see it both as a symptom of high glucose and as a side effect of medications commonly used in diabetes care and related conditions.
Causes: High blood sugar can reduce salivary gland function directly and promote dehydration through polyuria (excess urination). Many antihypertensives, diuretics, and antidepressants, drugs often prescribed alongside diabetes, also cause dry mouth. Radiation therapy to the head and neck and smoking further decrease salivary output.
Symptoms to watch for: a persistent thick or stringy feeling in the mouth, waking up thirsty at night, difficulty swallowing dry foods, cracked lips, a raw tongue surface, and fissures at the corners of the mouth (angular cheilitis). Some people notice trouble wearing dentures comfortably or a change in voice quality.
Risks: Saliva provides critical protective effects. When it’s reduced, we see a higher risk of dental caries (especially root caries), mucosal infections like candidiasis, bad breath, and faster plaque accumulation that can progress to gum disease. Dry mouth also contributes to a poorer quality of life: it affects taste, eating enjoyment, and sleep.
Practical notes: If dry mouth is new or worsening, we should check fasting and random blood glucose and review medications. Simple measures often help: increasing fluid intake (but not sugary drinks), sugar‑free lozenges or gum with xylitol to stimulate saliva, using a humidifier at night, and switching medications when appropriate. Prescription saliva substitutes or stimulants can be considered for severe cases after consulting a provider.
Burning Mouth, Taste Changes, And Swollen Or Fissured Tongue
Burning mouth sensation, altered taste (dysgeusia), and a swollen or fissured tongue are common oral complaints that we increasingly link to blood sugar dysregulation. These symptoms can be subtle at first and then become persistent, a cue that we shouldn’t ignore.
Burning mouth syndrome presents as a chronic, often bilateral burning or scalding pain of the oral mucosa without an obvious cause. In people with diabetes or prediabetes, neuropathy, damage to small sensory nerves, is a likely contributor. High glucose levels damage nerves over time, altering pain perception and temperature sensation. This can create a persistent burning sensation, even when the tissues look normal.
Taste changes include a metallic taste, reduced ability to taste sweet or salty, or a complete shift in flavor perception. These may result from neuropathy, dry mouth (which limits taste molecule transport), or recurrent oral infections.
A swollen, smooth, or fissured tongue can indicate nutritional deficiencies (like B12 or iron), dehydration, or chronic inflammation, all of which are more likely when blood sugar control is poor. Fissures (deep grooves) can trap food and microbes, increasing irritation or secondary infection. Glossitis (tongue inflammation) sometimes accompanies candidiasis, which we’ll cover more below.
When we evaluate these symptoms, we look for reversible contributors: adjusting glycemic control, correcting vitamin deficiencies, managing dry mouth, and treating infections. Symptom relief may come from topical analgesics, saliva stimulants, improved oral hygiene, and addressing neuropathic pain with medications or nonpharmacologic strategies as advised by a clinician.
Fungal Infections, White Patches, Slow‑Healing Sores, And Ulcers
Oral fungal infections, most commonly candidiasis, and mucosal lesions are more frequent and persistent in people with elevated blood sugars. Candida albicans thrives in a glucose-rich, dry environment and is a leading cause of white plaques and red, sore patches on the tongue and inner cheeks.
Classic presentations: pseudomembranous candidiasis (white curd‑like plaques that can be wiped off, revealing a red base), erythematous candidiasis (red, sore areas often on the tongue), and angular cheilitis (cracks at the mouth corners). Denture stomatitis is another Candida-related problem, where the tissue under a denture becomes inflamed and white.
Slow-healing sores and ulcers should raise concern. Hyperglycemia impairs wound healing through reduced blood flow, fewer immune cells in the wound area, and prolonged inflammation. Small bites, burns, or ulcerations that don’t resolve within 10–14 days deserve evaluation, persistent ulcers can become infected or, rarely, harbor malignancy, especially in patients with other risk factors like tobacco or heavy alcohol use.
Management: For candidiasis we typically recommend topical antifungals (nystatin suspension, clotrimazole troches) for localized disease: systemic agents (fluconazole) may be needed for extensive or recurrent infections. Addressing underlying dry mouth, optimizing blood sugar, improving denture hygiene, and removing prosthetic irritants are essential to prevent recurrence.
We must also rule out other causes of white lesions or ulcers, leukoplakia, lichen planus, aphthous ulcers, or early neoplastic changes. If a lesion doesn’t respond to standard therapy or looks suspicious (indurated, growing, bleeding), biopsy or specialist referral is appropriate.
Gum Disease, Bleeding Gums, And Receding Gums
Periodontal disease, inflammation and infection of the gums and supporting structures, has one of the clearest links to blood sugar problems. We often see more severe periodontitis, faster progression, and poorer responses to treatment in people with uncontrolled diabetes.
Mechanisms: Elevated glucose increases inflammatory mediators and impairs immune cell function, which together create a more aggressive bacterial biofilm and exaggerated tissue destruction. Microvascular changes reduce blood supply to the gums, limiting nutrient and immune access. Collagen metabolism is also altered in hyperglycemia, weakening the periodontal ligament and making tissues more prone to breakdown.
Signs we look for: gums that bleed easily when brushing or flossing, persistent bad breath, swollen or tender gums, gum recession (teeth appearing longer), deep pockets between teeth and gums on probing, and loosening teeth. Advanced disease can lead to bone loss and tooth loss if not treated.
The bidirectional relationship matters clinically: treating periodontal disease can improve glycemic control modestly, and better glucose management reduces periodontal inflammation. That’s why coordination between dental and medical care is important for people with diabetes.
Prevention and management: rigorous daily oral hygiene, brushing twice, flossing daily, and using interdental cleaners, plus regular professional cleanings are essential. Smoking cessation and good glycemic control drastically reduce risk. When periodontal disease is present, scaling and root planing, localized antibiotic therapy, and periodontal surgery in advanced cases are standard options. We recommend individualized recall intervals and close follow-up for people with diabetes because recurrence risk is higher.
When To See A Doctor, How It’s Diagnosed, And How Problems Are Managed
We shouldn’t wait when oral changes appear alongside symptoms of high blood sugar (increased thirst, frequent urination, fatigue) or if existing diabetes suddenly seems harder to control. Early evaluation helps prevent complications and identifies issues, like infection or nutritional deficiency, that require treatment.
Tests Your Provider Will Order
Primary care providers and dentists often work together. Expect basic testing to assess metabolic control and oral health status:
- Point-of-care or laboratory A1C to gauge average glucose over 2–3 months. An A1C ≥6.5% indicates diabetes: 5.7–6.4% suggests prediabetes.
- Random or fasting blood glucose when A1C isn’t available.
- Oral swabs or cultures for persistent white patches or suspected fungal infections.
- Complete blood count and nutrient testing (B12, ferritin/iron studies, folate) if glossitis or recurrent ulcers suggest deficiency.
- Imaging (dental X-rays) to evaluate bone loss when periodontal disease or unexplained dental pain is present.
- Biopsy referral for any mucosal lesion that’s persistent, indurated, or suspicious for dysplasia or malignancy.
Oral Signs That Require Urgent Care
Seek prompt evaluation if you notice:
- Rapidly spreading swelling, severe pain, difficulty breathing or swallowing, signs of deep-space infection.
- High fever with oral infections or signs of systemic spread.
- Bleeding that won’t stop after basic measures, especially if you’re on anticoagulants.
- A painful ulcer or lump that hasn’t improved after two weeks.
These situations may require antibiotics, urgent drainage, hospital-level care, or specialist intervention.
Practical Treatment Options And Self‑Care Steps
Management blends medical therapy, dental procedures, and lifestyle measures. Key actions we recommend:
- Optimize blood sugar control. Improved glycemic control reduces infection risk and speeds healing. Medication adjustments, dietary counseling, and diabetes education can all help.
- Treat infections promptly: topical or systemic antifungals for candidiasis: antibiotics for bacterial infections guided by clinical judgment: and removal or adjustment of ill‑fitting dental prosthetics.
- Intensify oral hygiene: supervise technique, consider electric toothbrushes, antiseptic mouth rinses (chlorhexidine short-term for periodontal flares), and daily interdental cleaning. Avoid alcohol-based mouthwashes if you have dry mouth.
- Manage dry mouth: sugar‑free lozenges, xylitol gum, saliva substitutes, hydration, and addressing causative medications with your clinician.
- Nutritional support: correct deficiencies (B12, iron, folate) if present: a balanced diet that supports glycemic goals and oral tissue health.
- Regular dental care: more frequent cleanings (often every 3–4 months) and early periodontal therapy when needed. Coordinate care: inform your dentist of diabetes status and medications.
- Pain and neuropathy management: topical anesthetics for painful mucosal lesions and systemic options (gabapentin, duloxetine) for neuropathic pain when appropriate and prescribed by a clinician.
By combining timely medical evaluation, targeted treatments, and daily self-care, we can significantly reduce complications and improve oral comfort and function.
Conclusion
Mouth and tongue changes are not trivial cosmetic issues, they’re often early or visible signs of metabolic dysfunction and can directly impact nutrition, quality of life, and systemic health. In 2026, with better screening tools and more integrated care, we have more opportunity than ever to use oral findings as a window into blood sugar control.
If you notice dry mouth, burning or taste changes, white patches or slow‑healing sores, bleeding or receding gums, or persistent tongue abnormalities, act early: check glucose control, see your dentist and primary care provider, and follow practical self-care steps. Our mouths give us clues: focusing and responding promptly, we protect oral health and support better overall metabolic outcomes.