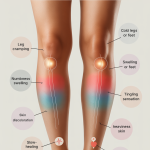
10 Symptoms in Your Legs That Could Signal Poor Circulation
The circulatory system is the body’s most essential transportation network, continuously delivering oxygen and nutrients to every tissue while removing metabolic waste. When this intricate system is compromised — particularly in the lower extremities — the consequences can range from mild discomfort to life-threatening complications. Poor circulation in the legs is not merely an inconvenience; it is frequently a signal of serious underlying vascular conditions such as peripheral artery disease (PAD), chronic venous insufficiency (CVI), deep vein thrombosis (DVT), or atherosclerosis.
According to the Cleveland Clinic, poor circulation occurs when obstacles in your blood vessels make it difficult for blood to reach the parts of the body farthest from the heart — most notably the legs and feet [^1]. Because the legs are the most distal extremities, they are often the first to manifest signs of compromised blood flow. Understanding these warning signs is critical, as early intervention can prevent severe complications including non-healing ulcers, infection, and in extreme cases, amputation.
This article examines 10 key symptoms in the legs that may indicate poor circulation, explaining the underlying physiology of each, the conditions they are associated with, and when to seek professional medical evaluation.
Understanding Poor Circulation: A Brief Overview
Poor circulation is not a disease in itself but rather a consequence of one or more underlying conditions that impair the normal flow of blood through the arteries and veins. The most common causes include:
| Cause | Mechanism | Associated Condition |
|---|---|---|
| Atherosclerosis | Plaque buildup narrows arterial walls | Peripheral artery disease (PAD) |
| Venous valve damage | Blood pools in veins due to faulty valves | Chronic venous insufficiency (CVI) |
| Blood clot formation | Clot partially or fully blocks a vessel | Deep vein thrombosis (DVT) |
| High blood pressure | Damages and weakens blood vessel walls | Hypertension-related vascular disease |
| Diabetes | Elevated glucose damages blood vessels | Diabetic peripheral vascular disease |
| Obesity | Increases pressure on veins and arteries | Venous hypertension, PAD |
| Smoking | Chemicals damage vessel lining | Accelerated atherosclerosis |
Risk factors for poor circulation include being over the age of 40, having diabetes, smoking, having high blood pressure, kidney disease, or a family history of vascular disease [^2]. Recognizing the early warning signs in the legs can prompt timely diagnosis and treatment, significantly improving long-term outcomes.
1. Leg Pain and Claudication
Perhaps the most clinically significant symptom of poor circulation is intermittent claudication — a pattern of leg pain that arises during physical activity and resolves with rest. The term derives from the Latin claudicare, meaning “to limp,” and it describes the characteristic discomfort that forces individuals to stop walking and rest before continuing.
Claudication typically manifests as cramping, aching, tightness, or a burning sensation in the calves, thighs, or buttocks. The pain is triggered by exercise because active muscles demand significantly more oxygen than at rest; when the arteries are narrowed by plaque or other obstructions, they cannot deliver sufficient blood to meet this demand. The resulting oxygen deficit causes lactic acid to accumulate in the muscles, producing the characteristic pain [^3].
According to the Mayo Clinic, claudication is the most common symptom of lower-extremity peripheral artery disease, and its severity can range from mild discomfort that occurs only after prolonged walking to debilitating pain that limits even minimal activity [^4]. In advanced cases, pain may persist even at rest — a condition known as critical limb ischemia, which represents a medical emergency requiring prompt intervention.
2. Numbness and Tingling (“Pins and Needles”)
A persistent sensation of numbness or tingling — often described as “pins and needles” — in the legs, feet, or toes is a common indicator of inadequate blood flow. Medically termed paresthesia, this sensation arises when nerves are deprived of the oxygen and nutrients they require to transmit signals properly.
Unlike the temporary tingling that occurs from sitting in an awkward position, circulation-related paresthesia tends to be recurrent, may occur at rest, and does not resolve simply by changing position [^1]. It can also be accompanied by a sensation of weakness or heaviness in the affected limb. This symptom is frequently associated with PAD, diabetic peripheral neuropathy, and Raynaud’s disease — a condition in which blood vessels in the extremities narrow in response to cold or stress.
It is important to distinguish between paresthesia caused by nerve compression and that caused by vascular insufficiency. A healthcare provider can help determine the root cause through appropriate diagnostic testing.
3. Persistent Coldness in the Legs or Feet
While occasional cold feet are entirely normal, persistently cold lower legs or feet — especially when one limb is noticeably colder than the other — can be a meaningful clinical sign. When blood flow to the extremities is reduced, less warm blood reaches the skin and tissues, resulting in a perceptible drop in temperature.
The Mayo Clinic specifically lists “coldness in the lower leg or foot, especially when compared with the other side” as a hallmark symptom of PAD [^4]. This asymmetry is particularly telling, as it suggests localized arterial obstruction rather than a systemic cause such as environmental cold. Raynaud’s disease can also cause episodes of extreme coldness in the toes and feet, often accompanied by color changes, in response to cold temperatures or emotional stress [^1].
4. Swelling of the Legs, Ankles, and Feet (Edema)
Peripheral edema — the accumulation of fluid in the tissues of the lower legs, ankles, and feet — is a hallmark sign of venous circulatory problems. When the veins cannot efficiently return blood to the heart, pressure builds up in the venous system, forcing fluid out of the blood vessels and into the surrounding tissues.
This type of swelling is commonly associated with chronic venous insufficiency (CVI), a condition in which the one-way valves inside the leg veins become damaged or weakened, allowing blood to flow backward and pool. The resulting edema is typically worse at the end of the day, after prolonged standing or sitting, and improves with leg elevation [^5]. Swelling can also be a sign of deep vein thrombosis (DVT), a potentially life-threatening condition in which a blood clot forms in a deep vein of the leg. DVT-related swelling is often accompanied by warmth, redness, and pain in the affected limb and requires immediate medical evaluation.
5. Skin Discoloration and Stasis Dermatitis
The skin of the legs can undergo a range of visible changes when circulation is impaired, making skin discoloration one of the most observable signs of vascular disease. Depending on the type and severity of the circulatory problem, the skin may appear:
- Pale or white, indicating severely reduced arterial blood flow
- Bluish or cyanotic, reflecting low oxygen levels in the blood
- Reddish-brown or bronze, a characteristic sign of venous stasis and iron deposits from leaking red blood cells
- Shiny or taut, often seen in advanced PAD where the skin becomes stretched and thin
A particularly important condition to recognize is stasis dermatitis (also called venous eczema), which develops when blood pools in the lower legs due to chronic venous insufficiency. The increased pressure causes fluid and red blood cells to leak into the surrounding skin tissue, triggering inflammation. The skin becomes discolored, itchy, scaly, and may eventually break down into open sores [^6]. Left untreated, stasis dermatitis can progress to venous ulcers, which are notoriously difficult to heal.
6. Slow-Healing Wounds and Leg Ulcers
One of the most serious consequences of poor circulation is the impaired healing of wounds. When the tissues of the lower legs and feet are chronically deprived of adequate blood flow, even minor cuts, scrapes, or pressure injuries can fail to heal properly and may evolve into chronic wounds known as leg ulcers.
There are two primary types of circulation-related leg ulcers. Venous ulcers, which account for the majority of chronic leg wounds, typically appear on the inner ankle and are caused by the chronic high pressure and fluid leakage associated with venous insufficiency [^7]. Arterial (ischemic) ulcers are caused by insufficient arterial blood supply and tend to appear on the toes, heels, or bony prominences of the foot. They are often more painful than venous ulcers and have a characteristic punched-out appearance with pale or necrotic tissue at the base.
Both types of ulcers are prone to infection and, if left untreated, can lead to cellulitis, osteomyelitis (bone infection), and in the most severe cases, gangrene requiring amputation. The presence of a non-healing wound on the leg or foot should always prompt urgent medical evaluation.
7. Varicose Veins and Visible Bulging Veins
Varicose veins are dilated, tortuous veins that become visible beneath the skin of the legs, often appearing as blue or purple rope-like cords. They are a direct manifestation of venous insufficiency, occurring when the valves within the veins fail to close properly, allowing blood to flow backward and pool, which causes the vein walls to stretch and bulge outward [^8].
While varicose veins are often considered a cosmetic concern, they can also cause significant physical symptoms, including an aching or heavy feeling in the legs, burning, throbbing, muscle cramping, and swelling in the lower legs. Symptoms are typically worse after prolonged periods of standing or sitting and may improve with leg elevation. More importantly, varicose veins are a visible marker of underlying venous disease that, if untreated, can progress to more serious conditions such as stasis dermatitis, venous ulcers, and DVT.
8. Hair Loss on the Legs
A less commonly recognized but clinically significant sign of poor circulation is the loss of leg hair. Hair follicles, like all living tissues, require a continuous supply of oxygen and nutrients delivered through the blood. When arterial blood flow to the legs is chronically reduced, the follicles are gradually starved of these essentials and eventually become dormant, leading to hair thinning or complete hair loss on the lower legs, ankles, and feet [^9].
This symptom is particularly associated with peripheral artery disease and may, in some patients, be one of the earliest or most prominent outward signs of the condition. According to the NHS, hair loss on the legs and feet is listed among the recognized symptoms of PAD alongside claudication and toenail changes [^10]. The distribution of hair loss — typically affecting the lower legs and dorsum of the foot — can help clinicians distinguish vascular-related hair loss from other dermatological causes.
9. Slow-Growing or Brittle Toenails
Just as hair follicles depend on adequate blood supply, so do the nail matrix cells responsible for toenail growth. When circulation to the feet is compromised, the nail matrix receives fewer nutrients and less oxygen, resulting in slow-growing, brittle, or thickened toenails [^11].
The Mayo Clinic notes slow-growing toenails as a recognized symptom of PAD, alongside hair loss and skin changes [^4]. In addition to slowed growth, the nails may become discolored (yellowish or brownish), develop ridges, or separate from the nail bed. These changes can also make the nails more susceptible to fungal infections, which are themselves more difficult to treat in the context of poor circulation. Toenail changes, while subtle, should be considered in the broader clinical picture, particularly when accompanied by other vascular symptoms.
10. Restless Legs
Restless leg syndrome (RLS) is characterized by an irresistible urge to move the legs, typically accompanied by uncomfortable sensations such as crawling, itching, burning, or aching. While RLS has multiple potential causes, there is a well-established association between the syndrome and venous insufficiency — a common cause of poor circulation in the legs.
Research suggests that impaired venous blood flow leads to the pooling of blood and the accumulation of metabolic waste products in the leg muscles, which can trigger or worsen the uncomfortable sensations of RLS [^12]. Studies have found that treating underlying venous disease in patients with RLS can significantly reduce the severity of their symptoms. The symptoms of RLS are typically worse at night or during periods of inactivity, which aligns with the pattern of worsening venous pooling when the legs are not elevated or actively used.
At a Glance: Summary of Symptoms
The following table provides a concise overview of the 10 symptoms, their primary cause, and the associated vascular condition.
| # | Symptom | Primary Cause | Associated Condition |
|---|---|---|---|
| 1 | Leg pain and claudication | Oxygen deficit in muscles during activity | Peripheral artery disease (PAD) |
| 2 | Numbness and tingling | Nerve oxygen deprivation | PAD, Raynaud’s disease, diabetes |
| 3 | Cold feet or lower legs | Reduced warm blood flow to extremities | PAD, Raynaud’s disease |
| 4 | Swelling (edema) | Venous blood pooling and fluid leakage | Chronic venous insufficiency, DVT |
| 5 | Skin discoloration | Reduced oxygenation, iron deposits | PAD, venous insufficiency, stasis dermatitis |
| 6 | Slow-healing wounds and ulcers | Impaired tissue oxygenation and repair | PAD, chronic venous insufficiency |
| 7 | Varicose veins | Faulty venous valves and blood pooling | Chronic venous insufficiency |
| 8 | Leg hair loss | Follicle oxygen and nutrient deprivation | PAD |
| 9 | Slow-growing or brittle toenails | Nail matrix nutrient deprivation | PAD |
| 10 | Restless legs | Venous blood pooling, waste accumulation | Chronic venous insufficiency |
When to Seek Medical Attention
Recognizing these symptoms is the first step; acting on them is equally important. You should consult a healthcare provider if you notice any of the symptoms described in this article, particularly if they are new, persistent, or worsening. Certain situations require immediate emergency care, including:
- Sudden, severe leg pain at rest, especially if accompanied by pallor or coldness of the limb
- A leg that is red, warm, swollen, and painful (possible DVT)
- A non-healing wound that shows signs of infection (increasing redness, warmth, pus, or odor)
- Sudden numbness or loss of feeling in a limb
Your doctor can diagnose poor circulation through a physical examination, ankle-brachial index (ABI) testing, Doppler ultrasound, or angiography. Treatment options range from lifestyle modifications — such as smoking cessation, regular exercise, and a heart-healthy diet — to medications, minimally invasive procedures, and surgery, depending on the severity and underlying cause of the circulatory problem [^2].
“Your entire health is intimately related with circulation. When circulation problems arise, your body often gives warning signs.” — Dr. Anahita Dua, MD, Vascular Surgeon, Massachusetts General Hospital [^13]
Early detection and treatment of poor circulation not only alleviates symptoms but can also significantly reduce the risk of life-threatening complications such as heart attack, stroke, and limb loss. Do not dismiss persistent leg symptoms as a normal part of aging — they may be your body’s way of alerting you to a serious, treatable condition.
References
[^1]: Cleveland Clinic. (2021, September 27). Poor Circulation: Symptoms, Causes and Treatment. https://my.clevelandclinic.org/health/diseases/21882-poor-circulation
[^2]: Temple Health. (2025, October 24). Poor Circulation: 7 Surprising Warning Signs. https://www.templehealth.org/about/blog/poor-circulation-7-surprising-warning-signs
[^3]: Mass General Brigham. (2025, October 20). Warning Signs of Poor Blood Circulation. https://www.massgeneralbrigham.org/en/about/newsroom/articles/signs-poor-blood-circulation
[^4]: Mayo Clinic. (2024, August 9). Peripheral Artery Disease (PAD): Symptoms and Causes. https://www.mayoclinic.org/diseases-conditions/peripheral-artery-disease/symptoms-causes/syc-20350557
[^5]: Cleveland Clinic. (2026, February 4). Edema. https://my.clevelandclinic.org/health/diseases/12564-edema
[^6]: Cleveland Clinic. (2022, October 28). Venous Stasis Dermatitis. https://my.clevelandclinic.org/health/diseases/24388-venous-stasis-dermatitis
[^7]: Hopkins Medicine. (n.d.). Venous Ulcers. https://www.hopkinsmedicine.org/health/conditions-and-diseases/venous-ulcers
[^8]: Mayo Clinic. (2024, February 6). Varicose Veins: Symptoms and Causes. https://www.mayoclinic.org/diseases-conditions/varicose-veins/symptoms-causes/syc-20350643
[^9]: USA Vascular Centers. (2025, November 11). Hair Loss on Legs: Warning Sign of PAD. https://www.usavascularcenters.com/blog/hair-loss-legs-might-vascular-problem/
[^10]: NHS. (n.d.). Peripheral Arterial Disease (PAD). https://www.nhs.uk/conditions/peripheral-arterial-disease-pad/
[^11]: USA Vascular Centers. (2025, November 13). Why Are My Toenails Not Growing? https://www.usavascularcenters.com/blog/toenails-can-tell-vascular-health/
[^12]: United Vein Centers. (2024, August 23). Restless Legs at Night: Could Venous Insufficiency Be the Cause? https://unitedveincenters.com/blog/restless-legs-at-night/
[^13]: Mass General Brigham. (2025, October 20). Warning Signs of Poor Blood Circulation. https://www.massgeneralbrigham.org/en/about/newsroom/articles/signs-poor-blood-circulation